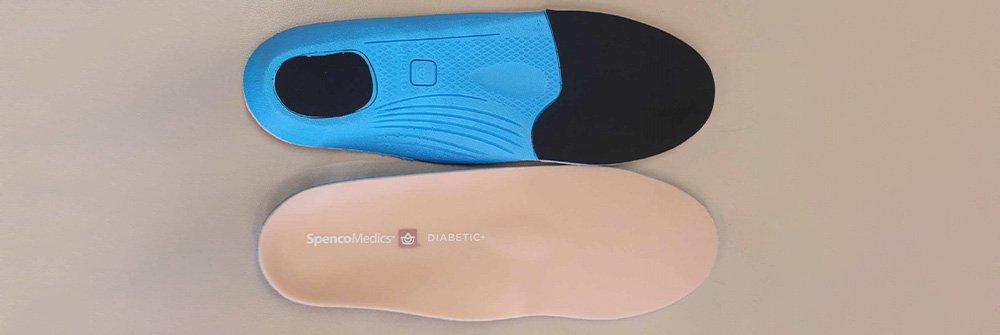
Diabetic foot care is a highly specialized area in footwear design. For people with diabetes, even minor pressure points or friction can lead to serious complications such as ulcers, infections, or long-term tissue damage.
That’s why insoles designed for diabetic foot care are not just about comfort—they are about protection, pressure distribution, and medical safety.
In this guide, we explain what truly matters when developing or sourcing insoles for diabetic users, including materials, structure, and key performance requirements.
Why Diabetic Feet Need Special Insoles
People with diabetes often experience:
-
Peripheral neuropathy (reduced sensation in feet)
-
Poor blood circulation
-
Higher risk of skin breakdown and ulcers
This means:
👉 Users may not feel pain from pressure or friction
👉 Small issues can quickly become serious medical problems
Standard insoles are not designed to address these risks.
Key Requirements for Diabetic Insoles
1. Pressure Redistribution
The most critical function of diabetic insoles is to reduce localized pressure.
High-pressure areas (such as the heel and forefoot) must be evenly distributed across the entire foot.
👉 Why it matters:
-
Prevents pressure ulcers
-
Reduces risk of tissue damage
2. Soft, Cushioning Materials
Diabetic insoles should use low to medium hardness materials to provide gentle cushioning.
Recommended materials:
-
Soft PU foam
-
Low-density EVA
-
Medical-grade cushioning foams
👉 Key goal:
Minimize impact and eliminate hard contact points
3. Seamless and Skin-Friendly Surface
The top layer must be:
-
Smooth
-
Seam-free
-
Non-abrasive
👉 Why:
Even small seams or rough textures can cause friction injuries for sensitive skin.
Common top covers include:
-
Fabric with antimicrobial treatment
-
Moisture-wicking materials
-
Soft microfiber layers
4. Moisture Management
Diabetic feet are more vulnerable to infection, especially in humid environments.
Insoles should:
-
Absorb or wick away moisture
-
Improve airflow
-
Reduce bacterial growth
👉 This helps maintain a healthy foot environment.
5. Proper Support Without Excessive Rigidity
While cushioning is important, diabetic insoles still need moderate support.
However:
❌ Too hard → creates pressure points
❌ Too soft → lacks stability
👉 The solution:
Balanced, multi-layer construction with controlled support zones.
6. Customization and Fit
Every diabetic foot is different.
Important factors:
-
Foot shape
-
Pressure distribution
-
Deformities (e.g., bunions, hammertoes)
👉 Custom or semi-custom insoles are often recommended.
Recommended Structure for Diabetic Insoles
A well-designed diabetic insole usually includes:
Top Layer (Comfort Layer)
-
Ultra-soft, skin-friendly
-
Moisture-wicking
-
Seamless surface
Middle Layer (Cushioning Layer)
-
Low to medium density
-
Shock absorption
-
Pressure redistribution
Base Layer (Support Layer)
-
Medium density
-
Provides stability
-
Maintains shape over time
👉 This multi-layer structure ensures both comfort and protection.
Materials Commonly Used
PU (Polyurethane)
-
Excellent cushioning
-
Long-lasting performance
-
Ideal for medical applications
EVA
-
Lightweight
-
Cost-effective
-
Suitable for basic diabetic insoles
Plastazote (Medical Foam)
-
Heat-moldable
-
Adapts to foot shape
-
Widely used in orthopedic and diabetic care
Common Mistakes to Avoid
1. Using standard insoles
Regular insoles do not provide adequate protection for diabetic feet.
2. Choosing materials that are too hard
This increases pressure points and risk of injury.
3. Ignoring moisture control
A damp environment promotes infection.
4. Lack of customization
A poor fit can lead to uneven pressure distribution.
Additional Features to Consider
High-quality diabetic insoles may also include:
-
Antibacterial treatments
-
Odor control technology
-
Heat-moldable customization
-
Removable pads for pressure offloading
These features further enhance safety and usability.
How to Choose the Right Supplier
For brands and importers, selecting the right manufacturer is crucial.
Look for suppliers who can:
-
Offer medical-grade materials
-
Provide multi-density design capabilities
-
Support customization and prototyping
-
Understand pressure distribution and foot biomechanics
Final Thoughts
Diabetic insoles are not just a comfort product—they are a protective solution designed to reduce risk and improve quality of life.
The most important factors include:
-
Pressure redistribution
-
Soft, skin-friendly materials
-
Moisture control
-
Proper structural support
For brands entering this segment, investing in the right design and materials is essential.
At Aybroad, we specialize in developing custom insole solutions tailored for different applications, including diabetic foot care. Our team works closely with clients to optimize material selection, structure, and performance based on real-world needs.
👉 Contact us today to discuss your diabetic insole project or request a sample.
 English
English  Español
Español  Português
Português  日本語
日本語  Français
Français  繁體中文
繁體中文  简体中文
简体中文